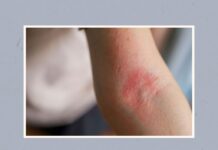
Eczema, or atopic dermatitis (AD), is a chronic inflammatory skin condition affecting millions worldwide. While commonly associated with childhood, it frequently persists into adulthood, impacting quality of life with persistent rashes, intense itching, and scaling skin. Approximately 8.9% of women and 5.7% of men in the U.S. experience AD, making it a significant health concern that often requires long-term management.
Зміст
Understanding Eczema’s Impact
The condition’s prevalence highlights the need for proactive management strategies, as flare-ups can be unpredictable and debilitating. Triggers vary widely, ranging from environmental factors like extreme temperatures to lifestyle choices, such as certain fabrics or stress levels. Without consistent care, eczema can disrupt daily life, causing discomfort, sleep disturbances, and social challenges.
Dermatologist Insights: Managing Triggers
Dr. Sandra Lee, a board-certified dermatologist and known as “Dr. Pimple Popper,” lives with mild-to-moderate eczema herself. She emphasizes the importance of diligent trigger avoidance: “I am diligent about avoiding trigger factors in my day-to-day life… steering clear of certain fabrics and environments.”
Common triggers include:
- Stress
- Temperature changes
- Harsh skincare products
- Fragrances
- Irritating fabrics (wool, polyester)
To better understand flare-up patterns, Dr. Lee recommends keeping a symptom diary. Tracking daily activities, diet, stress levels, and product usage can reveal connections over time, guiding more effective treatment plans.
Working with a Dermatologist
Effective eczema management requires collaboration with a healthcare professional. A dermatologist can confirm diagnosis, identify triggers, and recommend appropriate treatments.
“They can help you understand what might be contributing to your eczema and recommend treatments that are appropriate for you,” explains Dr. Lee. Clear communication and documentation of symptoms during appointments ensure a tailored approach.
Treatment Options: Beyond Steroids
For mild-to-moderate eczema not responding to traditional treatments, non-steroidal options like OPZELURA® (ruxolitinib) cream are available. OPZELURA is FDA-approved for short-term and non-continuous use in adults and children 2 years and older, offering relief without the long-term side effects sometimes associated with topical steroids.
Important Safety Considerations: OPZELURA carries risks, including serious infections, increased cancer risk, and cardiovascular events. It should not be used in combination with biologics, other JAK inhibitors, or strong immunosuppressants. Patients should discuss all medical history and potential side effects with their doctor before use.
A Dermatologist’s Personal Connection
Dr. Lee’s experience as both a dermatologist and patient shapes her approach to care. “Having eczema myself has helped me relate to my patients and approach care with more empathy.” This understanding drives her to personalize treatment plans, including prescribing OPZELURA when appropriate.
Resources and Support
Living with eczema is an ongoing learning process. Support is available through patient communities like the National Eczema Association (NEA), offering education, resources, and connections with others who understand the condition.
For more information on OPZELURA and patient experiences, visit MyMomentsOfClarity.com.
Ultimately, eczema management requires diligence, informed choices, and a strong partnership with a healthcare professional. By understanding triggers, working closely with a dermatologist, and exploring appropriate treatment options, individuals can regain control over their skin health and improve their quality of life.